By: Sarah Stein, MD, FAAD, FAAP & Sheilagh Maguiness, MD, FAAD, FAAP
Children with
eczema (atopic dermatitis) tend to get patches of dry, itchy skin. The itch can make it hard for them to
sleep. Plus, scratching can cause the rashes to get infected.
While there is no known cure for eczema, it can be treated so your child feels better. There are also ways to help your child avoid eczema flare-ups.
Eczema treatment strategies
Eczema treatments usually target four common problems: dryness, itching, irritated skin (inflammation) and infection.
Dryness: repairing & protecting the skin barrier
For children with eczema, the skin barrier isn't holding in water well. As a result, the skin becomes
dry and cracked, and is more likely to get infected. Dry skin is also very itchy.
Gentle skin care tips for children with eczema
Gentle skin care daily is important to improve the skin barrier. As part of this:
Give your child a bath (or shower) every day or every other day for 5-10 minutes in lukewarm water. No soap is needed, but a gentle non-soap cleanser can be used on the sweaty areas (armpits, neck, groin) and on the hands and feet. Use only fragrance-free, hypoallergenic cleansers. Avoid scrubbing your child's skin with anything rough. Don't use bubble bath in the bath water.
Pat your child's skin dry after the bath or shower. If your doctor has prescribed any topical medicines, apply these to the areas of rash (BEFORE applying any moisturizers).
Apply a moisturizer to the whole body immediately after bathing (while the skin is still damp) every day. This helps "lock in" the moisture of the water. The creamier the moisturizer, the better it will work. Ointments such as petroleum jelly or fragrance-free moisturizing CREAMS are good choices (lotions are thinner and less effective). Most importantly, find a moisturizer that your child likes to use. Moisturizers should be applied once or twice every day, even when the rash is gone.
Dress your child in soft fabrics like 100% cotton. Use mild, fragrance-free laundry detergents. Don't use fabric softeners or fabric sheets in the dryer. Minimize your child's exposure to things that are known to commonly be irritating to sensitive skin. This includes fragrance in products and in the air, for example, as well as smoke, dust, wool, and animal dander.
Reducing the itch of eczema
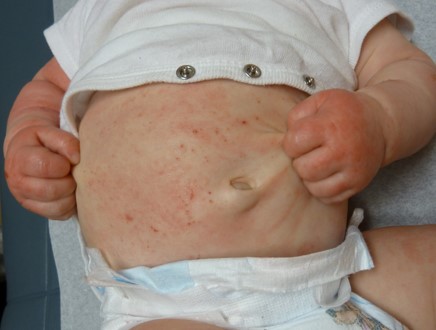
Gentle skincare as described above is the first step in making the skin feel less itchy.
Other ways to help reduce eczema itching:
Prevent scratching. Try to stop your child from scratching as much as possible since scratching can make the skin feel even more itchy. Scratching can also lead to open sores which can lead to skin infections. Keep your child's nails cut short. Wearing cotton gloves at night can also help.
Wet wrap treatments. Apply wet wraps AFTER bathing and applying topical medicines and moisturizers. Here's how:
Apply prescribed medicine to areas of rash and apply moisturizer to surrounding skin.
Soak a pair of pajamas or onesies in warm water.
Wring out the pajamas until they are damp and not dripping.
Put the damp pajamas on your child, with dry pajamas on top.
Make sure the room is warm or provide a warm blanket, so your child doesn't feel cold.
Keep the wet wraps on for at least half an hour, or leave them on overnight.
After removing the wet wraps, reapply moisturizer.
Healing irritated skin & rashes
To help calm an inflamed eczema rash and support skin healing, your child's doctor may recommend topical treatments.
-
Topical steroid medicines ("steroids" or "cortisones") are applied to the skin to heal irritated eczema rashes (inflammation). These prescription medications are very effective and safe when used appropriately. They are usually used twice a day when the rash is flaring. Topical steroids come in different strengths and forms (such as lotions, ointments, creams, gels, and oils). Your doctor will help you find the right combination for your child's skin.
Non-steroid eczema medicines (examples include tacrolimus ointment, pimecrolimus cream, crisaborole ointment, roflumilast cream, ruxolitinib cream, and tapinarof cream) have been increasingly developed in recent years. These medications also help heal irritated eczema rashes using different active ingredients than steroids. They can be helpful on mild to moderate eczema and on delicate areas of skin, like the eyelids, armpits and groin.
Managing & preventing skin infections
Bacteria and viruses can make eczema rashes worse, and it's important to watch for signs of infection.
Look for
oozing, crusting, pus bumps, blisters or a worsening rash that is not getting better with your usual treatments. Be sure to talk to your doctor if you think your child's skin is infected. Infections may require antibiotic or antiviral medicines.
Diluted bleach baths for eczema: a how-to guide
Soaking in a tub with a small amount of bleach added to the water 2-3 times per week can help prevent skin infections. Diluted bleach baths, which are similar to swimming in a chlorinated pool, are easy to do at home:
Add 1/2 cup of plain household bleach (sodium hypochlorite) OR 1/3 cup of concentrated household bleach to a full tub of lukewarm bathwater and stir the water to dilute the bleach. Make sure you use PLAIN bleach; splash-free or scented bleach products are not effective and could lead to more irritation.
If using an infant tub, use 2 tablespoons of bleach to a full tub of water.
Have your child soak in the bath for 10-15 minutes. Try to soak the entire body. Since the bath is like a swimming pool, it is safe to get your child's face and scalp wet as well. For babies and young children, use
touch supervision to avoid drowning as you would during regular bath time.
Rinse the dilute bleach water off at the end of the bath. Then, after pat-drying the skin, apply eczema medicine to areas of rash and a moisturizer all over.
New treatments for eczema
-
Biologic therapies ("biologics") are medicines that target the part of the immune system that is causing the irritated skin rash. Biologic medications are given by injection. Dupilumab was the first biologic therapy approved by the U.S. Food & Drug Administration (FDA) for the treatment of eczema in children ages 6 months and up. Other biologics, including tralokinumab, lebrikizumab and nemolizumab, recently were approved for use in children.
-
Another class of medicines known as
JAK inhibitors, also work to treat eczema by regulating the skin immune system. These medicines are given orally and some (upadacitinib and abrocitinib for example), have been tested and approved in children.
These newer medication types can be very helpful for moderate to severe eczema that is not well controlled with topical medicines and gentle skin care.
Talk to your doctor to learn more about these treatment options.
When can I stop treatment for an eczema rash?
Once your child's skin is no longer itchy and the areas of rash are smooth and soft, you can start to use the medicines less often.
Does skin discoloration from eczema go away?
It is common for the skin to be discolored after the rash flare heals, but the color will naturally normalize over time. However, since eczema is an ongoing skin problem, it is important to continue your routine of gentle skin care and use of moisturizers every day to minimize future flares and infections.
How can I prevent future eczema flares?
Gentle daily skin care, as described above, is one of the most important things you can do to prevent future eczema flares. Talk with your doctor about a daily routine that is best for your child.
Avoiding triggers is also important to prevent future flares of eczema. Eczema triggers are different for different children. Some parents and physicians may consider allergy testing to further identify triggers that can be avoided. Some
triggers include:
In rare cases, certain foods can flare an eczema rash. If you think this might be the case,
talk to your doctor before trying any restrictive dietary changes.
Remember
Keep in mind that your child's eczema may still flare despite your best efforts. Eczema is an ongoing skin problem that requires patience and consistent skin care. Don't hesitate to reach out to your child's pediatrician or
pediatric dermatologist for support.
More information
About Dr. Stein
 Sarah Stein, MD, FAAD, FAAP, a member of the American Academy of Pediatrics Section on Dermatology, is Associate Professor and Director of Pediatric Dermatology for UChicago Medicine.
Sarah Stein, MD, FAAD, FAAP, a member of the American Academy of Pediatrics Section on Dermatology, is Associate Professor and Director of Pediatric Dermatology for UChicago Medicine. About Dr. Maguiness
 Sheilagh Maguiness, MD, FAAD, FAAP, is director of pediatric dermatology at the University of Minnesota in Minneapolis. Dr. Maguiness is a past Executive Committee Memeber and Education Chair of the American Academy of Pediatrics Section on Dermatology. She is a mom to two boys and is originally from Canada.
Sheilagh Maguiness, MD, FAAD, FAAP, is director of pediatric dermatology at the University of Minnesota in Minneapolis. Dr. Maguiness is a past Executive Committee Memeber and Education Chair of the American Academy of Pediatrics Section on Dermatology. She is a mom to two boys and is originally from Canada.
|
|
*Image provided by Sheilagh Maguiness, MD, FAAD, FAAP