By: Christine Lauren, MD, FAAP & Sean Reynolds, MD, FAAP
A child's toddler and preschool-age years are filled with new experiences, like a first playdate or first tricycle. Often by around age 5, however, a less-than-fun first also may pop up: a child's first cold sore.
Here's what parents need to know about cold sores in children, including how to treat and manage them.
What are cold sores?
Cold sores
(also called fever blisters or oral herpes) start as small blisters that form around the lips and mouth. They sometimes appear on the chin, cheeks, and nose, too. After a few days, the blisters usually begin to ooze, then form a crust and heal completely in one to two weeks.
Do colds cause cold sores?
Despite their name, cold sores actually have nothing to do with colds. In children, cold sores are usually caused by the herpes simplex virus type 1 (HSV-1). Genital herpes is usually caused by a different strain, herpes simplex virus type 2 (HSV-2), although both virus strains can cause sores in any part of the body.How do cold sores spread?
Cold sores are highly contagious. They can spread through saliva, skin-to-skin contact, or by touching an object handled by someone infected with the virus.
Most people are first exposed to HSV between ages 1 and 5 years of age; more than half of people in the United States are infected with it by the time they become adults. Beyond the uncomfortable sores that the virus can cause, HSV is usually harmless.
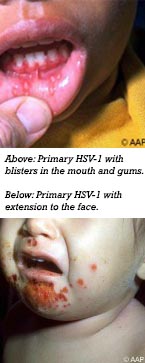
Symptoms of primary HSV
When a child develops a cold sore for the first time (also called primary HSV), the blisters often spread beyond the lips to the mouth and gums. A child may also have a fever, swollen and tender lymph glands, sore throat, irritability and drooling. Sometimes symptoms are so mild, though, parents may not even notice any of them.
Can cold sores cause other problems?
If HSV spreads to the eyes
The virus from cold sores can spread to the eyes, which can lead to
HSV keratitis, an eye infection. The infection usually heals without damaging the eye, but more severe infections can lead to scarring or blindness.
If HSV spreads to a newborn
HSV is dangerous to babies under 6 months of age, especially newborns within the first few months of life.
Parents or relatives with active cold sores should be especially careful not to kiss babies. Signs that a baby may have been infected with HSV include one or more small skin blisters or sores on their skin. Low grade fever may also be seen. These symptoms can occur 2 to 12 days after HSV exposure. If concerning skin lesions occur, contact your pediatrician.
If your child has eczema
If your child has eczema (atopic dermatitis) and develops a cold sore, they may develop widespread blisters and sores on their skin. This is called eczema herpeticum. Children with this condition can get sick and, in some cases, require hospital admission. If your child has eczema and develops new blisters or sores, call your pediatrician.
Do cold sores come back?
After a child's first cold sore, the virus settles into bundles of nerve cells in the body—causing no symptoms unless it activates and travels back up to the skin's surface.
While the virus remains in the body for the rest of your life, outbreaks of cold sores vary. Some children may never get another cold sore, while others may have multiple outbreaks a year. When the virus does reactivate, cold sores tend to form again at the same spot near the mouth or wherever on the skin they first appeared.
Signs of a cold sore flare up
The first signs of a flare up include tingling, itching, or burning. Parents might notice their child keeps touching or scratching a spot of skin that then starts to swell and redden before the sores form.
Common cold sore triggers
Once a child is infected with the cold sore virus, it is more likely to return during times when the body's immune system is rundown, or the skin becomes irritated from other causes.
Common cold-sore triggers for children previously exposed to the virus include:
Fatigue and stress
Exposure to intense sunlight, heat, cold or dryness
Injuries to or breaks in the skin
Illness (such as colds or the flu)
Dehydration and poor diet
Fluctuating hormones (during a teen's menstrual periods, for example)
How to treat & manage cold sores in children
Although there is currently no cure for cold sores, the good news is that they heal on their own over a few days to a week or two. Medications are usually not necessary during an outbreak. Parents can protect against spreading sores, help relieve pain during a flare-up, and try to avoid possible triggers.
Stop the spread of HSV.
Try to prevent your child from scratching or picking at cold sores. This can spread the virus to other parts of the body, such as fingers and eyes, as well as to other children who touch toys and other objects they play with. Wash hands and clean toys regularly.
During a cold sore flare-up, don't let your child share drinks or utensils, towels, toothpaste or other items to avoid spreading the infection. Also, wash items such as towels and sheets in hot water after use.
Children usually can go to child care or school with an active infection. But your pediatrician may suggest keeping them home if they drool a lot or are having their very first HSV outbreak.
See
When to Keep Your Child Home from Child Care for more information.
If your child participates in sports that involve skin-to-skin contact such as
wrestling, they should sit out during an active cold sore infection. Make sure mats and other equipment are cleaned regularly after use.
Help soothe cold sore pain.
Apply ice or a warm washcloth to the sores to decrease pain from a cold sore.
Chilled or icy treats such as smoothies may be soothing to sore lips and can help avoid dehydration.
Avoid giving your child acidic foods during a cold sore outbreak (e.g., citrus fruits or tomato sauce). These can irritate cold sores.
If your child's cold sores continue to hurt—especially if he or she does not want to eat or drink because of mouth pain—ask your pediatrician about giving a pain reliever such as
acetaminophen or
ibuprofen. Your pediatrician may also suggest a medicine to shorten the outbreaks by a day or two.
Avoid cold sore triggers.
Strong sun exposure and sunburn can bring on a cold sore outbreak. So be sure your child uses sun protection for skin and lips before heading outdoors.
Make sure your child gets enough sleep, exercise and eats a well-balanced diet.
Help your child manage
stress, which can increase the likelihood of cold sore outbreaks.
When to see your pediatrician about a cold sore
During your child's first cold sore infection: This is especially recommended if your child has a known difficulty in fighting infections or a chronic skin condition such as
eczema. Your child should see their pediatrician if they are drinking less during the infection as this may lead to dehydration.
If your newborn develops a blister-like rash or fever: This could be symptoms of a dangerous
neonatal herpes simplex infection.
If there are sores or blisters near your child's eyes: HSV is the most common cause of corneal infections.
If your child develops a headache, combined with confusion, seizure or fever during a cold sore outbreak: This could signal a dangerous brain infection caused by the virus, including
meningitis or encephalitis.
If the sores do not heal on their own within seven to 10 days: Your pediatrician might want to rule out a secondary bacterial infection and/or any other medical condition.
If skin surrounding cold sores becomes reddened, swollen or feels hot to the touch: This may be signs of a secondary bacterial infection.
If your child gets frequent cold sores: Children with more than five or six outbreaks a year might benefit from antiviral medications. Talk to your pediatrician about a prescription if your child's outbreaks are frequent.
More information
About Dr. Lauren
 Christine Lauren, MD, FAAP, is an Associate Professor of Dermatology and Pediatrics at Columbia University Vagelos College of Physicians and Surgeons and New York-Presbyterian Hospital. She is currently a member of the Executive Committee of the Section of Dermatology of the AAP. She serves as an Associate Designated Institutional Official at New York-Presbyterian where she engages with residents and fellows across their academic campuses. Christine Lauren, MD, FAAP, is an Associate Professor of Dermatology and Pediatrics at Columbia University Vagelos College of Physicians and Surgeons and New York-Presbyterian Hospital. She is currently a member of the Executive Committee of the Section of Dermatology of the AAP. She serves as an Associate Designated Institutional Official at New York-Presbyterian where she engages with residents and fellows across their academic campuses.
|
About Dr. Reynolds
 Sean Reynolds, MD, FAAP, is an Assistant Professor of Pediatrics at the University of Missouri-Kansas City School of Medicine and a Clinical Assistant Professor of Internal Medicine at the University of Kansas School of Medicine. Sean attended medical school in Ireland at the University College Cork School of Medicine before moving to the U.S. to complete his pediatrics residency at Boston Children's Hospital, followed by his dermatology residency at Brown University. He completed his medical training with a fellowship in pediatric dermatology at the University of California San Francisco. He joined the Division of Dermatology as faculty at Children's Mercy in 2020 where he serves as the Director of Resident Education and is the Associate Fellowship Director for their Pediatric Dermatology Fellowship Program. Sean Reynolds, MD, FAAP, is an Assistant Professor of Pediatrics at the University of Missouri-Kansas City School of Medicine and a Clinical Assistant Professor of Internal Medicine at the University of Kansas School of Medicine. Sean attended medical school in Ireland at the University College Cork School of Medicine before moving to the U.S. to complete his pediatrics residency at Boston Children's Hospital, followed by his dermatology residency at Brown University. He completed his medical training with a fellowship in pediatric dermatology at the University of California San Francisco. He joined the Division of Dermatology as faculty at Children's Mercy in 2020 where he serves as the Director of Resident Education and is the Associate Fellowship Director for their Pediatric Dermatology Fellowship Program.
|